Scientists have confirmed, in the largest study of its kind to date, that bacteria—not fungi—are the primary culprit behind Auto-Brewery Syndrome (ABS), a rare medical condition in which patients experience symptoms of intoxication after eating, despite having consumed no alcohol.
The research team analyzed stool samples from 22 patients diagnosed with ABS, as well as from their healthy partners living in the same household. The results showed that two specific bacterial species were significantly more abundant in individuals with the syndrome, reinforcing findings from a previous 2019 study, according to Science Alert. Although the number of participants was limited, it represents a notable cohort of rigorously controlled cases whose gut bacteria produced high levels of ethanol in laboratory cultures.
Rarely diagnosed
ABS is rarely diagnosed, and there is still no scientific consensus on how best to treat it, the researchers note. The study was led by infectious disease specialist Elizabeth Hohmann of Massachusetts General Hospital and gastroenterologist Bernd Schnabl of the University of California, San Diego.
“Many patients seek medical care only to be dismissed as secret drinkers and leave without a diagnosis,” the study states.
Elevated ethanol levels in their bodies often cause liver damage, as well as serious social, family, and legal problems.
Two “culprit” bacteria
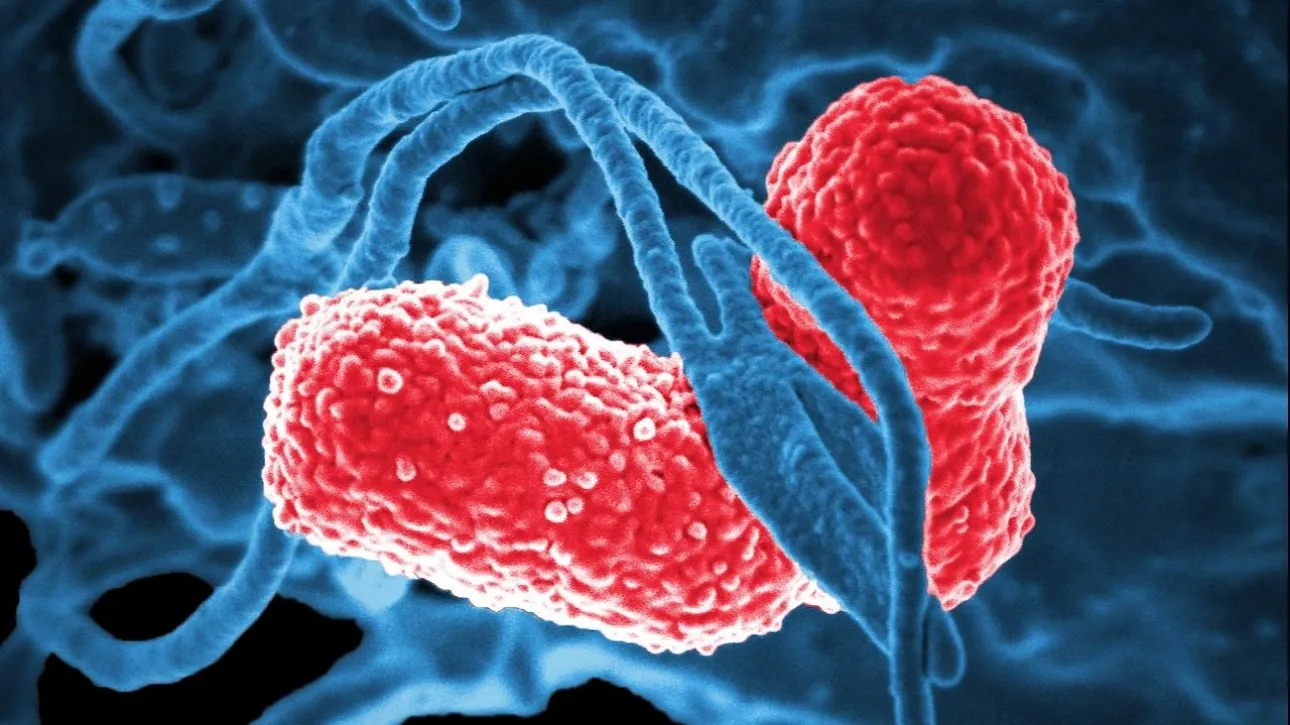
The new study was prompted by a surge of calls received by microbiologist Jing Yuan of the Beijing Institute of Pediatrics from patients desperate to be tested for ABS. It was 2019, and Yuan—who did not participate in the current study—had just published research pointing to the bacterium Klebsiella pneumoniae as a potential cause of ABS. She referred callers to Schnabl, who went on to organize the new study, recently published in the journal Nature Microbiology.
By comparing the gut microbiome of patients with that of their cohabiting partners, the researchers effectively controlled for environmental and dietary factors. They found that bacteria from patients during flare-ups—when symptoms of intoxication occurred—produced more ethanol than bacteria from patients in remission or from healthy individuals, a finding that correlated with blood alcohol levels.
The ethanol-producing bacteria K. pneumoniae and Escherichia coli were more prevalent in ABS patients, with E. coli showing a particularly marked increase during flare-ups.
In one notable case, a patient showed dramatic improvement after two fecal microbiota transplants from a healthy donor, remaining in remission for more than 16 months. The patient’s family reported that their behavior had “essentially returned to normal.”
The findings suggest that patient relief may come from interventions that promote bacteria capable of metabolizing ethanol—through diet, probiotics, or fecal transplants—while not ruling out a role for fungi in certain cases. The researchers also note that patients exhibited extreme imbalances in their gut microbiome, and that other studies have linked microbial ethanol production in the gut to diabetes and fatty liver disease.